High Risk Complex Coronary Angioplasty
Overview
Coronary angioplasty is one of the most effective and widely used treatments for restoring normal blood flow to the heart. When a coronary artery becomes narrowed or completely blocked due to cholesterol deposits or plaque buildup, the heart muscle does not receive enough oxygen-rich blood. This condition can lead to chest pain, breathing difficulty, fatigue, or even a major heart attack. Coronary angioplasty helps open these narrowed arteries, reduce symptoms, and prevent future cardiac complications.
At Good Heart Clinic, coronary angioplasty is performed using advanced catheter-based technology and high-precision stent systems. The procedure is minimally invasive and offers quick recovery, making it an excellent option for patients experiencing heart blockages. The goal of angioplasty is simple: to restore smooth blood flow and improve the long-term health of your heart. This procedure plays a vital role in emergency situations, especially during heart attacks, where every minute counts.
Coronary Angioplasty in Pune
If you are looking for advanced coronary angioplasty in Pune, Good Heart Clinic provides expert evaluation and interventional cardiology care for patients with blocked coronary arteries.
Heart angioplasty in Pune is a minimally invasive procedure used to restore blood flow in narrowed or blocked arteries and prevent heart attacks.
What is a Coronary Angioplasty?
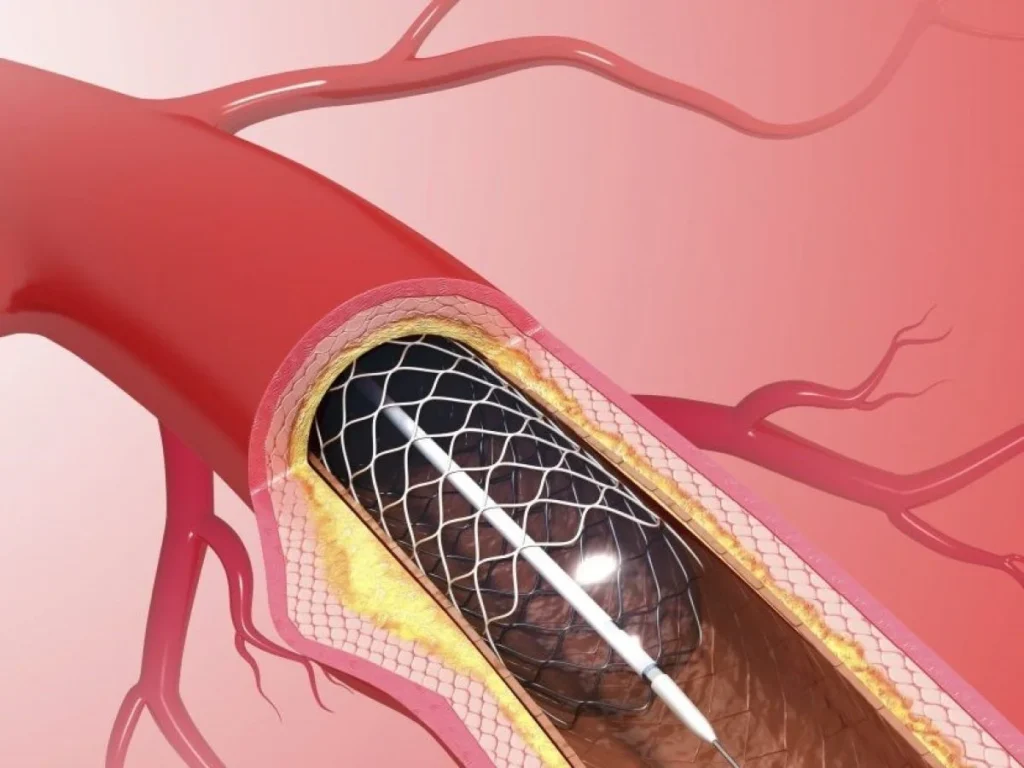
Coronary angioplasty, medically known as Percutaneous Coronary Intervention (PCI), is a procedure used to treat blocked or narrowed coronary arteries. It involves opening the artery using a balloon and often placing a stent to keep it open. The stent acts as a support structure that ensures the artery remains wide enough for blood to flow freely.
This treatment is commonly recommended for patients who have:
- Significant coronary artery blockages
- Recurrent chest pain (angina)
- Symptoms that do not improve with medication
- Abnormal results on tests such as ECG, Stress Test, or Angiography
- A history of heart attack or high-risk cardiac conditions
Coronary angioplasty is considered the cornerstone of modern cardiac care because it is minimally invasive, highly effective, and offers immediate improvement in symptoms.
Time Taken for the Procedure
Coronary angioplasty timing varies depending on the complexity of your blockages and whether you’re having an emergency or planned procedure.
The procedure
30 minutes to 2 hours, depending on how many arteries need treatment and the complexity of your blockages.
Recovery and observation
4-8 hours minimum, often requiring overnight stay.
Total hospital time
Most patients stay overnight for observation, especially if stents were placed. Some may stay 1-2 nights depending on their condition and response to treatment.
Symptoms
Chest Pain
When chest discomfort persists even after medication, it may indicate significant artery blockage.
Breathlessness on Minimal Activity
Difficulty breathing during simple tasks is often a sign of reduced heart function due to narrowed arteries
Abnormal ECG, Stress Test, or Angiography Findings
If diagnostic tests show reduced blood flow to the heart muscle, angioplasty is suggested to prevent further damage to the heart.
Heart Attack (Myocardial Infarction)
In emergency cases, angioplasty is performed immediately to open the blocked artery and save heart tissue from permanent damage.
Recurrent Chest Pain
These classic heart symptoms indicate possible coronary artery blockages, requiring timely angioplasty to reduce the risk of a major cardiac event.
Fatigue, Dizziness
Such symptoms may occur when blood flow to the heart is severely compromised, prompting the need for angioplasty.
Poor Response to Heart Medications
If symptoms continue despite prescribed heart medicines, angioplasty may be necessary to correct the underlying blockage.
Stress-Triggered Discomfort
If anxiety or emotional strain brings on chest or heart-related sensations.
Benefits
Immediate Relief from Chest Pain
Prevents Heart Damage
Quick and Minimally Invasive Treatment
Improves Long-Term Heart Health
Preparations
Proper preparation ensures that the procedure is safe and successful. Your doctor will provide complete guidance before the procedure.
Before the Day of Your Procedure:
On the Day of Your Procedure:
What Does the Procedure Involve?
Arrival at the Catheterization Lab:
You’ll be taken to the cardiac catheterization laboratory, or “cath lab”—a specialized room equipped with imaging equipment and monitoring systems. The environment may seem intimidating with its technology, but the staff will help you feel comfortable.
The team will help you lie on a padded procedure table. Monitoring equipment will be attached to track your heart rate, blood pressure, oxygen levels, and heart rhythm throughout the procedure. An IV line will be started if not already in place.
Anesthesia and Comfort Measures:
You’ll remain awake during angioplasty, but you’ll receive sedation medication through your IV to help you relax. Most patients describe feeling calm and drowsy but able to respond to instructions.
Your doctor will thoroughly clean the insertion site—your wrist or groin—with antiseptic solution. Local anesthetic will be injected to numb the area completely. You’ll feel a brief sting or burning sensation from the numbing medicine, but this quickly subsides.
Catheter Insertion and Navigation:
Your doctor makes a small puncture in your artery and inserts a thin plastic sheath. Through this sheath, a catheter is carefully threaded through your blood vessels. You won’t feel the catheter moving inside your body.
Using X-ray guidance visible on monitors throughout the room, your doctor navigates the catheter to your heart. Contrast dye is injected to make your coronary arteries visible, helping identify the exact location of blockages. You may feel a warm, flushing sensation when dye is injected—this is completely normal and passes quickly.
Opening the Blockage:
Once your doctor has located the blockage, a specialized guidewire is carefully advanced through the blocked area. This thin wire serves as a track for the balloon catheter.
The balloon catheter is then positioned precisely at the blockage. When everything is in place, your doctor inflates the balloon, typically several times, for 30-60 seconds each time. As the balloon inflates, it compresses the plaque against the artery wall and stretches the artery open.
You might feel brief chest discomfort or pressure during balloon inflation—this is normal as blood flow is temporarily blocked. The discomfort disappears immediately when the balloon is deflated. Tell your doctor about any discomfort you experience.
Stent Placement:
In most cases, your doctor will place a stent to keep the artery open. The stent is mounted on the balloon catheter. When the balloon inflates, it expands the stent, pressing it firmly against the artery wall. The balloon is then deflated and removed, but the stent remains permanently in place.
Your doctor may use special imaging called intravascular ultrasound (IVUS) or optical coherence tomography (OCT) to ensure the stent is properly positioned and fully expanded.
Multiple Blockages:
If you have blockages in multiple arteries, your doctor may treat them during the same procedure or schedule separate sessions depending on complexity and your condition.
Final Checks and Completion:
After the stent is placed, more contrast dye is injected to confirm blood is flowing freely through the treated artery. Your doctor verifies the blockage has been successfully opened and the stent is secure.
Once satisfied with the results, all catheters are carefully removed. The puncture site is closed using manual pressure, a closure device, or a compression band depending on the location.
What You Might Experience:
- Pressure at the insertion site during catheter placement
- Warmth or flushing when contrast dye is injected
- Brief chest discomfort during balloon inflation
- Awareness of lights and equipment around you
- Voices of the medical team working together
- Generally minimal pain throughout
The entire procedure typically feels much less dramatic than you might expect.
What Follows the Procedure?
After angioplasty, you will be shifted to a recovery area where nurses and doctors closely monitor your heart rate, blood pressure, and pulse.
First Week at Home:
- Activity restrictions: Avoid heavy lifting, pushing, or pulling anything over 10 pounds for at least one week. Don’t participate in strenuous exercise or sports. You can walk and perform light daily activities. Take stairs slowly and rest when needed.
- Insertion site care: Keep the area clean and dry. You can shower after 24-48 hours, but avoid soaking in baths, hot tubs, or swimming pools for one week. Watch for signs of infection like redness, warmth, swelling, or drainage.
- Driving: Wait at least 48 hours before driving, or longer if you’re taking narcotic pain medications or feeling weak.
- Return to work: Most people return to work within 3-7 days if their job doesn’t involve heavy physical labor. Discuss timing with your doctor based on your specific situation.
- Hydration: Drink 8-10 glasses of water daily for the first few days to help your kidneys flush out the contrast dye.
Warning Signs
- Bleeding from the insertion site that doesn’t stop with 10-15 minutes of firm pressure
- A growing lump, significant swelling, or bruising at the insertion site
- Pain, numbness, tingling, or coldness in the arm or leg where the catheter was inserted
- Chest pain or pressure, especially if similar to your pre-procedure symptoms
- Shortness of breath or difficulty breathing
- Irregular heartbeat or heart palpitations
- Fever over 100.4°F (38°C)
- Unusual weakness or dizziness
- Any concerns about your incision site
Frequently Asked Question (FAQs)
No. Angioplasty is a minimally invasive cardiac procedure, not an open-heart surgery. A thin catheter is inserted through the wrist or groin, and a balloon is used to widen the artery. A stent is then placed to keep the artery open. Patients often resume normal activities within a few days.
A stent is a small metal mesh tube placed inside the blocked artery during angioplasty. It acts like a support system that keeps the artery open, allowing smooth and continuous blood flow. Stents significantly reduce the chances of the artery narrowing again.
No. Coronary angioplasty is not painful. Local anesthesia is used at the insertion site, so patients may feel slight pressure but no pain. Most people remain awake and comfortable during the PCI procedure.
Yes. Coronary angioplasty is considered one of the safest and most successful cardiac procedures. It is performed by experienced cardiologists in a well-equipped cath lab. Serious complications are rare, and patients are carefully monitored throughout the procedure.
Yes. By opening blocked arteries and restoring blood flow, angioplasty reduces the risk of future heart attacks. Placing a stent helps prevent the artery from narrowing again, offering long-term protection for heart health.

